Measles Outbreak 2024: The Resurgence Of A Preventable Threat
Could a disease that the United States declared eliminated over two decades ago be staging a dangerous comeback? The unsettling answer is yes. Across the nation, measles outbreaks are no longer rare anomalies but a troubling recurrence, with case counts climbing and public health officials sounding alarms. From a massive outbreak in South Carolina to explosive clusters on college campuses in Florida, the highly contagious virus is exploiting gaps in community immunity. This comprehensive guide dives deep into the current measles situation, explains why vaccination rates are critical, and provides essential information on symptoms, exposure alerts, and what you must do to protect yourself and your family.
What Exactly Constitutes a Measles Outbreak?
The Centers for Disease Control and Prevention (CDC) defines a measles outbreak as three or more confirmed cases that are epidemiologically linked, meaning they are related through person-to-person transmission or a common exposure location. This threshold is crucial because a single imported case is expected occasionally due to international travel, but multiple related cases signal community transmission has begun. Most outbreaks in the United States have historically been small, typically comprised of six people or fewer, and often confined within a household or a close-knit social circle. These contained clusters are usually extinguished quickly through contact tracing and post-exposure prophylaxis for vulnerable individuals.
However, the current landscape is different. The defining characteristic of today's outbreaks is not just their size but their persistence and geographic spread. When an infectious person moves through a population with low vaccination coverage, the virus finds a susceptible pathway. The basic reproduction number (R0) for measles is estimated to be between 12 and 18, meaning one infected person can transmit the virus to 12-18 others in a fully susceptible population. This extreme contagiousness makes even small pockets of unvaccinated individuals a tinderbox for explosive spread.
- Kent Ehrhardt Height Weight Net
- Ekane And Her Bd
- Melinda Gates Boyfriend
- Beyoncé Age Unraveling The Timeline Of A Global Icon
The Current U.S. Landscape: South Carolina and Florida Lead a Surge
The current measles situation in the U.S. is being driven by two major, concurrent outbreaks that have shattered years of relative quiet. The most severe is a large outbreak in South Carolina that began in late 2023. As of the latest state health department reports, this single outbreak has recorded 962 cases across six counties, with the vast majority occurring in unvaccinated children. This makes it the largest outbreak in the state's history and the most significant in the nation in over 30 years.
To combat this crisis, a mobile clinic offering measles and flu vaccinations was deployed, with a sign announcing its services on February 6, 2024, in Spartanburg, South Carolina—a visible symbol of the emergency response. The scale of the South Carolina outbreak prompted a federal response, with a dozen public health experts from the CDC and other agencies arriving to assist the state health department. It’s important to note this team is not coming from the CDC's Atlanta headquarters as a routine deployment, but as a specialized emergency support mission to contain the largest U.S. measles outbreak in decades.
Simultaneously, Florida is grappling with its own significant outbreak, centered at Ave Maria University near Naples. This measles outbreak at Ave Maria University has led to at least 66 confirmed cases in Collier County, with 48 cases directly tied to the university campus. Statewide, Florida has reported 92 measles cases across 11 counties, making it the second-largest outbreak cluster in the country. This college campus outbreak marks the largest wave of measles infections on an American university campus in recent history. A student at Ave Maria University publicly detailed his symptoms—high fever, cough, and a characteristic rash—highlighting the personal toll of this outbreak. With over 40 people falling ill at the university, public health experts fear that college campuses may become new hotspots for measles transmission due to dense living conditions and potential gaps in vaccination records among students from diverse geographic and ideological backgrounds.
- Norman Wiegand
- What Is Wrong With Simon Cowells Son
- Who Is Michelle Payne Married To
- Little House On The Prairie Reboot Everything We Know About Netflixs Modern Reimagining
Nationally, the CDC's weekly update confirms that 976 of the U.S. cases were reported across 26 states. This widespread distribution underscores that no region is immune when vaccination rates falter. Health officials consistently remind the public that measles is highly contagious and can cause serious illness, resulting in hospitalizations and, in severe cases, death. The resurgence is a stark reversal of a major public health victory.
How Measles Spreads and Why Vaccination is Non-Negotiable
Measles is a viral disease transmitted through respiratory droplets and airborne particles. An infected person can spread the virus up to four days before the characteristic rash appears and for about four days after. The virus can remain infectious in the air or on surfaces for up to two hours, meaning you can contract measles in a room even after an infected person has left. This extreme contagiousness is why herd immunity—where a high percentage of the community is immune—is essential to protect those who cannot be vaccinated, such as infants or immunocompromised individuals.
The MMR vaccine (measles, mumps, rubella) is remarkably effective. Two doses are about 97% effective at preventing measles, and one dose is about 93% effective. Widespread vaccination with a highly effective vaccine is what halted the ongoing spread of measles in the U.S. more than 20 years ago, leading to its declaration of elimination in 2000. However, recent outbreaks have flared in over 20 U.S. states, leading to hospitalizations and at least two deaths, primarily among unvaccinated individuals.
A pivotal study from a measles outbreak in the Netherlands in 1999 provides a critical lesson. Researchers found that more cases were detected in vaccinated people living in mostly unvaccinated communities than in unvaccinated people in highly vaccinated communities. Why? In areas with high vaccination rates, herd immunity protects even the unvaccinated. But in communities with low vaccination coverage, the virus circulates widely, and because no vaccine is 100% perfect, the small percentage of vaccinated individuals who lack full immunity can become infected when exposed to high viral loads. This study powerfully demonstrates that vaccination is not just a personal choice; it's a community responsibility. Your decision not to vaccinate doesn't just put you at risk—it increases exposure danger for everyone around you, including those who are vaccinated.
Recognizing Measles: Symptoms, Contagion, and Who's Most at Risk
Understanding measles symptoms is vital for early detection and containment. The illness typically progresses in two stages:
- Initial Stage (Days 1-10): High fever (often reaching 104°F/40°C), cough, runny nose (coryza), and red, watery eyes (conjunctivitis). The fever can last 4-7 days and may spike as other symptoms worsen.
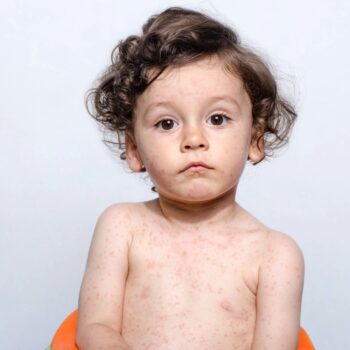
- Rash Stage (Days 10-14): A characteristic red, blotchy rash appears, typically starting at the hairline and spreading down the face, neck, trunk, arms, legs, and feet. The rash may be itchy and lasts 5-6 days. Koplik spots—tiny white lesions on the inside of the cheeks—may appear 2-3 days before the rash and are a telltale sign for clinicians.
Who is most at risk? The highest risk groups include:
- Unvaccinated infants and children: They have no pre-existing immunity.
- Pregnant women: Measles can cause miscarriage, premature birth, or low birth weight.
- Immunocompromised individuals: Those with weakened immune systems from cancer treatment, HIV/AIDS, or other conditions may not be able to receive the live vaccine and are at severe risk for complications.
- Adults who missed vaccination: Some adults may have only received one dose or none, especially if born after 1957 but before widespread vaccination.
Complications are common and can include diarrhea, ear infections, pneumonia (the most common fatal complication), encephalitis (brain swelling), and a rare but fatal degenerative brain disease called subacute sclerosing panencephalitis (SSPE) that can occur years later. Hospitalization occurs in about 1 in 4 cases, and death can occur in 1-2 per 1,000 cases, with young children and malnourished individuals at highest risk.
Public Health in Action: Exposure Alerts and Emergency Metrics
To quickly notify the public of potential measles exposure sites and prevent further spread, health authorities at local, state, and federal levels issue measles exposure alerts. These alerts identify specific locations, dates, and times when an infectious person was present while contagious. For example, an alert might state: "An individual with confirmed measles visited County Library Branch A on January 15, 2024, from 2:00 PM to 5:00 PM." The goal is to alert anyone who was there during that window to monitor for symptoms for 21 days (the maximum incubation period) and contact their healthcare provider or health department immediately if symptoms develop. These alerts are a critical tool for breaking the chain of transmission.
Behind the scenes, public health agencies use standardized case definitions to track outbreaks accurately. A case refers to a measles infection reported in a resident of a specific jurisdiction, like North Carolina (NC). These metrics do not include cases reported in travelers who are just passing through; they focus on resident infections to gauge community spread. The date used for outbreak dashboards is the date symptoms began. If that date is not available, the specimen collection date or the report date is used as a proxy. This consistency allows for accurate epidemic curves and trend analysis. More detailed information on the official CDC case definition is available in a PDF document for healthcare professionals.
The Bigger Picture: Lagging Vaccination Rates and Community Vulnerability
The resurgence of measles is not a mystery; it is directly linked to declining vaccination rates among children in certain communities. The U.S. has seen a rise in vaccine hesitancy and refusal, fueled by misinformation, religious exemptions, and philosophical beliefs. The national MMR vaccination rate among kindergarteners has slipped slightly below the 95% herd immunity threshold in some states and communities. When vaccination rates drop below this critical level, the virus can find enough susceptible hosts to sustain transmission.
This creates a dangerous patchwork of immunity. Outbreaks are not randomly distributed; they cluster in areas with concentrated under-vaccination, often linked to specific schools, religious groups, or geographic regions. The South Carolina outbreak is a prime example, with health officials noting that most of the 950 people across six counties are unvaccinated children. Similarly, the Ave Maria University outbreak occurred in a community where vaccination rates may have been lower than the state average. These outbreaks serve as a warning: as long as measles circulates globally (and it does, with large outbreaks in Europe, Asia, and Africa), imported cases will continue to land in the U.S. and ignite fires in communities with dry tinder—the unvaccinated.
What You Can Do: Practical Steps for Protection
Measles is highly preventable, and your actions matter. Here is a clear action plan:
- Verify Your Vaccination Status: Ensure you and your children have received two doses of the MMR vaccine. The first dose is typically given at 12-15 months, and the second at 4-6 years. Adults born after 1957 who lack evidence of immunity (vaccination records, laboratory confirmation, or birth before 1957) should get vaccinated, especially if traveling internationally or working in healthcare, education, or childcare.
- Heed Exposure Alerts: If you receive a measles exposure alert for a location you visited, check your vaccination records. If you are unvaccinated or unsure, contact your doctor immediately. Post-exposure prophylaxis with the MMR vaccine within 72 hours or immune globulin within 6 days can prevent or lessen the disease.
- Recognize Symptoms Early: Be vigilant for the fever, cough, runny nose, and rash sequence. If you suspect measles, call your healthcare provider before arriving to avoid exposing others in the waiting room.
- Isolate if Infected: If diagnosed with measles, stay home and away from others for four days after the rash appears to prevent spread.
- Advocate for Community Immunity: Talk to friends and family about the importance of vaccination. Support school and workplace policies that require up-to-date immunizations.
Conclusion: A Preventable Disease, A Collective Responsibility
The return of measles outbreaks to the United States is a sobering public health setback. What we are witnessing is not a failure of medical science but a failure of collective memory and action. The MMR vaccine is a safe, effective, and time-tested shield. The outbreaks in South Carolina and Florida are not isolated incidents; they are symptoms of a broader vulnerability created by slipping vaccination rates.
The data is clear: in communities with high vaccination coverage, measles cannot gain a foothold. The 1999 Netherlands outbreak study taught us that even vaccinated individuals are safer when everyone around them is vaccinated. Recent outbreaks in over 20 U.S. states prove that the virus will exploit any gap in our defenses.
The message from health authorities is unequivocal: measles is highly contagious and can cause serious illness resulting in hospitalizations and death. But it is also highly preventable. The path forward is straightforward—renew our commitment to vaccination, trust in evidence-based science, and respond swiftly to exposure alerts. The legacy of a measles-free America depends on the choices we make today, not just for ourselves, but for our communities and the most vulnerable among us. The time to act is now, before the next exposure alert lands in your inbox.
- Miracles From Heaven The True Story That Inspired The Film And Transformed Millions
- Fav Princess Peach Filter Uncensored
- Your Ultimate Guide To Following The Minnesota Vikings News Schedules And Insider Access
- Azzi Fudd Biological Father

New school year, new measles outbreak? - ABC News
Measles outbreak - Childrens Liver Disease Foundation

Measles Outbreak 2025: U.S. Cases Hit 33-Year High | BASS Medical Group