Rhian Butlin Unnecessary Hysterectomy: A Story Of Misdiagnosis, Trauma, And A Different Cancer Battle
What happens when a life-altering medical procedure is performed based on a devastating mistake? For Rhian Butlin, a 32-year-old mother of two from the UK, this isn't a hypothetical question—it's her reality. Her journey from excruciating pain to an unnecessary hysterectomy, and then to a far more complex cancer diagnosis, exposes the profound fragility of the diagnostic process and the irreversible consequences of medical error. This is the story of Rhian Butlin's unnecessary hysterectomy, a case that serves as a stark warning about patient advocacy, the limits of medical certainty, and the resilience required to fight a battle that was wrongly declared from the start.
Biography and Personal Details
Before diving into the medical ordeal, it's important to understand the woman at the center of this story. Rhian Butlin is a 32-year-old British woman and a mother of two young children. In September 2024, her life took a dramatic turn when she sought help for severe health issues.
| Attribute | Detail |
|---|---|
| Full Name | Rhian Butlin |
| Age | 32 |
| Nationality | British |
| Family | Mother of two children |
| Key Event | Underwent an unnecessary hysterectomy in December 2024 following a misdiagnosis of ovarian cancer. |
| Actual Diagnosis | Later discovered to have a different, rare, and aggressive cancer (specific type not publicly named) that had metastasized. |
| Current Status | Fighting stage 4 cancer; speaking out to raise awareness. |
The Beginning: "Excruciating" Pain and Initial Dismissal
The First Signs of Trouble
Back in September 2024, Rhian Butlin went to the doctors with what she described as "excruciating" abdominal pain. This wasn't a mild discomfort; it was a debilitating symptom that disrupted her daily life as a mother. For many women, persistent pelvic or abdominal pain is a significant red flag, often leading to investigations for conditions like endometriosis, ovarian cysts, or, in more alarming cases, tumors.
- Bernie Taupin S Net Worth Fact Career Awards
- Who Is Nicolás Balmaceda Pascal The Brother Redefining Fame Away From Hollywood
- George Strait Death
- Azzi Fudd Biological Father
The First Misstep: Dismissal as PCOS
Tragically, Rhian's severe pain was initially dismissed. She was initially misdiagnosed with PCOS (Polycystic Ovary Syndrome), a common hormonal disorder. While PCOS can cause pain and cysts, the severity of Rhian's symptoms should have prompted deeper investigation. This initial misdiagnosis represents a critical failure in listening to the patient's lived experience and using pain intensity as a vital diagnostic clue. It delayed the identification of the true, more serious problem lurking beneath.
The Cancer Scare: A Tumor is Found
Escalation and Further Testing
As Rhian's pain persisted or worsened, further medical imaging—likely an ultrasound or CT scan—revealed the presence of a tumor on her ovary. This finding immediately escalated the situation from a chronic condition management to a potential cancer crisis. The discovery of an ovarian mass is one of the most frightening moments for any patient, as ovarian cancer is often diagnosed at a late stage and carries a poor prognosis.
The Devastating Verdict
Based on the imaging and preliminary assessments, doctors delivered the life-shattering news: they believed the tumor was ovarian cancer. This diagnosis, in itself, is a traumatic event, triggering a cascade of fear, urgent consultations with oncology teams, and discussions about aggressive treatment plans to save the patient's life. For Rhian, this meant preparing for a fight against a disease she believed she had.
- Riley Mar Lewis Leaked
- Gordan Ramsey Height
- Is Patrick Warburton Conservative
- Bianca Dos Santos The Mastermind Behind The 2009 Borges Family Kidnapping
The Unnecessary Hysterectomy: A Life-Changing Error
The Decision for Major Surgery
The standard, often life-saving, treatment for confirmed or highly suspected ovarian cancer is a hysterectomy—the surgical removal of the uterus and cervix—along with the removal of both ovaries and fallopian tubes (a bilateral salpingo-oophorectomy). Given the suspected diagnosis, this extensive surgery was presented as a necessary, urgent step to eradicate the cancer. In December 2024, Rhian Butlin underwent this major procedure.
The Scope of the Unnecessary Surgery
The surgery was even more extensive than a standard hysterectomy for ovarian cancer. During the operation, surgeons also removed her appendix and the lining of her bowel (likely a partial colectomy or omentectomy). These are common additions when cancer is suspected, as the disease can spread to these areas. Every organ removed was a permanent, life-altering loss, performed under the grave assumption it was necessary to save her life from ovarian cancer. The physical recovery from such a surgery is arduous, involving weeks or months of healing, significant lifestyle changes, and the immediate onset of surgical menopause if her ovaries were removed.
The Shocking Truth: A Different Cancer Emerges
The Post-Surgical Pathology Report
The definitive truth about any cancer diagnosis comes from the pathology report after the tumor is surgically removed and examined under a microscope. This is the gold standard. When Rhian's removed tissues were analyzed, the results delivered a second, even more shocking blow: the diagnosis was wrong. The tumor was not ovarian cancer.
The Real, and More Complex, Diagnosis
Instead, the pathology revealed that Rhian actually had another kind of cancer. The key sentences specify this other cancer has since metastasized, meaning it has spread to other parts of her body. The fact that it had metastasized by the time of discovery is a critical and tragic detail. It suggests the cancer was aggressive and had been growing for some time, possibly during the period she was being treated for the wrong condition. While the specific type isn't named in the provided sentences, it is described as "rare" and "aggressive" and is now at stage 4, meaning it is incurable but treatable. The unnecessary hysterectomy did nothing to combat this real cancer, which continued to progress unchecked.
The Aftermath: Trauma, Metastasis, and an Apology
The Double Trauma of Misdiagnosis
Rhian Butlin's experience constitutes a profound medical trauma. First, she endured the psychological torture of believing she had a deadly cancer. Then, she underwent a mutilating surgery that robbed her of her reproductive organs and parts of her digestive system, all based on that belief. Finally, she learned the surgery was for nothing—the cancer she actually had was still present, had spread, and was now stage 4. This sequence represents an immense betrayal of trust and a cascade of physical and emotional devastation. The unnecessary trauma and setbacks in her treatment are immeasurable.
The Metastasis: A Critical Complication
The fact that her actual cancer has metastasized is perhaps the most dire consequence. The delay in correctly diagnosing and treating her real cancer—while resources and focus were on the wrong condition—allowed it to advance to a late stage. This directly impacts treatment options, prognosis, and quality of life. It transforms her battle from potentially curable (if caught earlier) to a chronic, life-limiting management of stage 4 disease.
Doctors' Apology and Rhian's Decision to Speak Out
Following the revelation of the misdiagnosis, doctors later apologized to Rhian. While an apology is a necessary first step, it cannot reverse the surgery or the cancer progression. Rhian has chosen to channel her experience into action. She is speaking out publicly, using her platform (#bestmornings is mentioned in one key sentence, suggesting a media appearance or social media campaign) to share her story. Her goal is to highlight the dangers of diagnostic errors, the importance of patient vigilance, and the need for systemic checks in healthcare.
The Sobering Reminder: Diagnostic Process Complexity
A Fragile and Imperfect System
As one key sentence concludes, Rhian Butlin’s case is a sobering reminder of how fragile and complex the diagnostic process can be. Medicine is not an exact science. Diagnoses rely on interpreting tests, imaging, and symptoms, all of which can be ambiguous or misleading. Ovarian masses, in particular, can be challenging to characterize without surgical pathology. However, this complexity does not absolve the system from striving for accuracy and having robust safeguards.
The Chain of Errors
This case likely involved multiple points of failure:
- Symptom Interpretation: Dismissing severe pain as PCOS.
- Diagnostic Imaging: Misinterpreting the nature of the ovarian tumor on scans.
- Multidisciplinary Communication: Potential gaps between radiology, gynecology, and oncology teams.
- The "Surgical Diagnosis" Fallacy: Proceeding to radical surgery based on high suspicion rather than definitive pre-operative proof, a common but risky practice in oncology.
Broader Implications: Patient Advocacy and Systemic Change
The Imperative of Informed Consent
Rhian's story underscores the critical importance of informed consent. Patients must be fully aware of the certainty (or uncertainty) of a diagnosis before consenting to irreversible, life-changing surgery. Were the risks of a misdiagnosis and the possibility of finding something else clearly communicated? Did she understand that the pathology might reveal a different story? True informed consent requires transparency about diagnostic confidence levels.
The Role of Patient Advocacy
Rhian Butlin's experience is a powerful lesson in patient advocacy. She advocated for herself by returning with persistent pain, but the system failed her initially. Patients must be encouraged to:
- Trust their instincts about their own bodies.
- Seek second opinions for serious diagnoses, especially before major surgery.
- Ask direct questions: "What is the certainty of this diagnosis? What else could it be? What are the risks if we are wrong?"
- Request to see imaging and ask for detailed explanations.
Systemic Safeguards Needed
On a systemic level, this case calls for:
- Mandatory Second Reads: For pre-operative cancer diagnoses, especially for radical surgeries, requiring a second radiologist or pathologist to review imaging/biopsy.
- Multidisciplinary Tumor Boards: Ensuring complex cases are discussed by a full team of specialists before definitive treatment plans are made.
- Enhanced Diagnostic Protocols: For ambiguous ovarian masses, considering less invasive staging procedures or neoadjuvant (pre-surgical) chemotherapy in certain cases to confirm diagnosis before full surgery.
- Culture of Transparency: Creating non-punitive environments where diagnostic errors are openly reviewed to prevent recurrence.
Connecting the Dots: From PCOS to Stage 4
The narrative arc from the key sentences is chilling in its progression:
- A young mother seeks help for excruciating abdominal pain.
- Her pain is dismissed as PCOS.
- A tumor is found, leading to a diagnosis of ovarian cancer.
- She undergoes an unnecessary hysterectomy with removal of appendix and bowel lining.
- Pathology reveals the misdiagnosis—she had a different, rare, aggressive cancer.
- This real cancer had metastasized to stage 4 during the delay.
- Doctors apologized for the error.
- She is now speaking out about her ordeal.
This sequence highlights the catastrophic domino effect of a single diagnostic error. The initial dismissal allowed the real cancer to grow. The confident but wrong ovarian cancer diagnosis triggered a massive, unnecessary surgical intervention. The true cancer, untreated, progressed to metastasis.
Actionable Steps for Patients Facing a Serious Diagnosis
Based on the lessons from Rhian Butlin's case, here are crucial steps for anyone facing a potential cancer or major surgery diagnosis:
- Get All Records: Obtain copies of all imaging reports (CT, MRI, ultrasound), blood work, and clinical notes.
- Seek a Second Opinion: This is not a sign of distrust but of prudence. Take your records to a different hospital or a specialist center.
- Ask About Biopsy: For any solid tumor, a tissue biopsy (a small sample) is the only way to confirm cancer and its type before major surgery. Insist on understanding if a biopsy was done and what it showed.
- Question the Certainty: Ask your doctor, "On a scale of 1-10, how certain are you of this diagnosis? What are the other possibilities?"
- Understand the Surgery: Before consenting, ask: "Is this surgery being done because we are 100% sure it's cancer X, or because we are treating it as if it is cancer X? What will we learn from the surgery that we don't already know?"
- Request a Tumor Board Review: For complex cancers, ask if your case has been or will be presented to a multidisciplinary tumor board.
- Document Everything: Keep a journal of symptoms, questions, and answers.
Conclusion: A Fight That Shouldn't Have Been Necessary
Rhian Butlin's story is a heartbreaking paradox. She underwent a brutal, unnecessary surgery intended to save her from one cancer, only to discover she had a different, aggressive cancer that had silently advanced to stage 4. The unnecessary hysterectomy did not cure her; it compounded her trauma while her real enemy grew unchecked. Her experience forces us to confront the uncomfortable truth that within the sophisticated world of modern medicine, diagnostic errors can and do happen, with devastating, irreversible consequences.
Rhian is not just a victim of a mistake; she is now a warrior in a battle that was made infinitely harder by that mistake. Her voice, raised in platforms like #bestmornings, is a vital beacon for change. It reminds us that behind every test result and diagnosis is a human being whose life, body, and trust are on the line. The fragile and complex diagnostic process demands humility from practitioners and vigilance from patients. Rhian Butlin’s journey is a sobering call to build a healthcare system where such catastrophic errors are not just apologized for, but systematically prevented. Her resilience in speaking out ensures that her unnecessary trauma will not be in vain, potentially saving others from a similar fate of being treated for the wrong enemy while the right one wages war within.
{{meta_keyword}} rhian butlin unnecessary hysterectomy, ovarian cancer misdiagnosis, medical error, patient advocacy, informed consent, hysterectomy complications, metastatic cancer, diagnostic error, second opinion, medical trauma, gynecologic oncology, UK healthcare, stage 4 cancer, rare cancer, surgical mistake, patient rights.
- Monica Barbaro Husband Connor Tillman
- Roxanne Perez Net Worth
- Belle Delphine Family
- Who Is Nicolás Balmaceda Pascal The Brother Redefining Fame Away From Hollywood

Lawsuit: Hysterectomy Unnecessary - CBS News

Unnecessary Hysterectomy- Hormones Matter
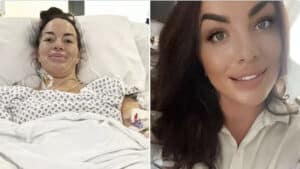
Rhian Butlin has womb removed after wrong cancer diagnosis